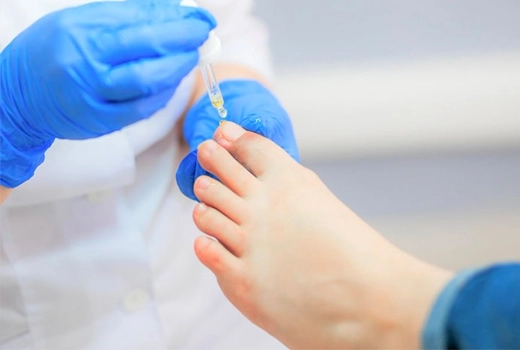
Diabetic foot is one of the most serious and common complications caused by diabetes. This condition can lead to disability, limb loss, and injuries, while also requiring long-term hospitalisation. However, this complication is actually a preventable condition.
Diabetes is a chronic metabolic disorder that prevents the body from properly using carbohydrates, fats, and proteins. This disease occurs as a result of insulin deficiency or insulin ineffectiveness. Diabetes requires continuous medical care and can cause damage to many organs in the body. High blood sugar leaves harmful effects on many systems, especially the nerves and vascular system. As a result of these effects, serious complications such as diabetic foot disease may develop.
Nervous system damage is one of the common consequences of diabetes and is called “diabetic neuropathy.” The nervous system consists of motor, autonomic, and sensory nerves that ensure the functioning of our body. When motor nerves are affected, muscle functions are impaired, leading to deformities in the feet and toes. This condition can cause deformities such as hammer toe, claw toe, and foot drop. Such deformities create a basis for further damage to the foot structure.
Damage to the autonomic nerves disrupts the functioning of the skin’s sebaceous glands, causing the skin to dry and crack. As a result, cracks form on the skin of the feet, making them vulnerable to infections. In addition, impairment of the nerves that regulate blood circulation prevents sufficient blood flow to the feet. This makes it difficult for the tissues to be nourished and hinders the healing of wounds.
Damage to the sensory nerves causes loss of sensation. Due to this loss, a diabetic patient may not notice cuts, burns, or other injuries on their feet. If these unnoticed injuries are left untreated, they can progress and lead to serious infections and tissue loss.
In addition to nerve damage, diabetes also causes vascular blockages due to the damage high blood sugar levels inflict on blood vessel walls. Blocked vessels cannot deliver enough blood to the tissues, and this accelerates tissue damage.
The combination of factors such as diabetic neuropathy, poor blood circulation, and loss of sensation makes the feet vulnerable to wound formation. Wounds that develop in diabetic feet do not heal as easily as in healthy individuals. When these wounds become infected, if left untreated, they can lead to serious consequences such as limb loss. This entire condition defines “Diabetic Foot.”
Approximately 25% of individuals with diabetes are at risk of developing a diabetic foot ulcer during their lifetime. This condition significantly reduces quality of life and leads to problems such as lower limb amputations and high treatment costs. Research shows that the three-year life expectancy of individuals who experience diabetes-related limb loss is only 50%. This rate is worse than the life expectancy of many types of cancer.
For this reason, it is critically important that wounds developing on the feet of diabetic patients are treated in a timely and proper manner. Scientific studies emphasise that diabetic foot patients should be treated in specialised wound care centres.
The most important causes of diabetic foot are diabetic neuropathy and damage to the vascular system. However, the underlying factor behind these conditions is high blood sugar and the inability to keep it under control. For this reason, the first step in diabetic foot treatment is regulating the patient’s blood sugar.
If the patient is using oral diabetes medications, switching to insulin therapy may be necessary. For patients already on insulin, it is important to reassess and appropriately adjust insulin doses. Without bringing blood sugar under control, it is not possible for diabetic foot treatment to progress effectively.

In diabetic patients, vascular problems occur in two main ways. The first is vascular blockages that develop due to damage caused by diabetes in the walls of the main arteries. The second is diabetes-related damage to the autonomic nervous system, which affects the muscles in the vessel walls and prevents blood from reaching the extremities.
With current treatment methods, it is generally not possible to reverse damage to the autonomic nervous system. Therefore, the primary goal in diabetic patients is to treat blockages in the main arteries.
For this purpose, a technique called the endovascular method is used. Similar to coronary angioplasty, the vessels are opened with the help of a catheter using a balloon or stent. If the problem cannot be resolved with this method, more extensive surgical interventions such as bypass surgery are attempted to address the vascular blockage. These approaches play an important role in the management of diabetic vascular problems.
Neuropathy associated with diabetic foot is a condition caused by nerve damage, leading to numbness in the foot. High blood sugar levels damage the nerves, causing patients to fail to notice injuries and allowing wounds to worsen. The most important step in neuropathy treatment is controlling blood sugar levels. This is a critical requirement to slow the progression of nerve damage and to alleviate existing symptoms.
In cases of painful neuropathy in diabetic foot, medication is used for pain management. Anticonvulsants, antidepressants, and topical pain relievers, together with vitamin B supplements, are commonly used to support nerve function. In addition, regular exercise and the use of appropriate orthoses are important to support wound healing in the foot and to improve circulation.
A multidisciplinary approach is required in treatment. To promote the healing of diabetic foot ulcers, pressure-relieving methods on the wound should be combined with neuropathy treatment. Physiotherapy and, when necessary, surgical interventions may also be included in the treatment plan to improve blood circulation and accelerate wound healing. With regular check-ups and appropriate treatment methods, complications caused by neuropathy and diabetic foot can be minimised.
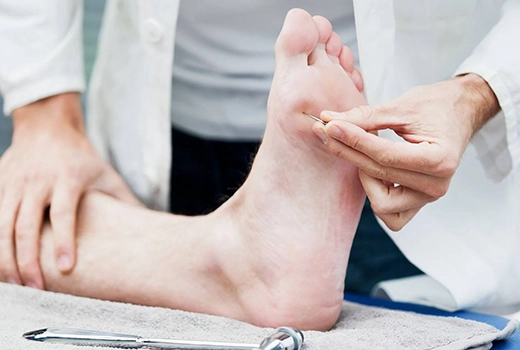
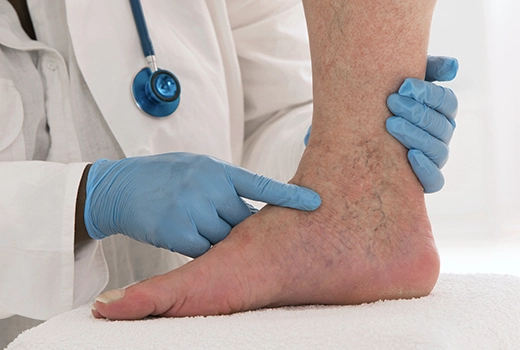
In the healing of diabetic foot ulcers, the presence of healthy capillaries that ensure sufficient oxygen and nutrient supply to the tissues is of vital importance. Diabetes-related vascular damage reduces blood circulation, preventing wound healing and increasing the risk of infection. Therefore, one of the main goals of treatment is to promote the formation of new healthy capillaries.
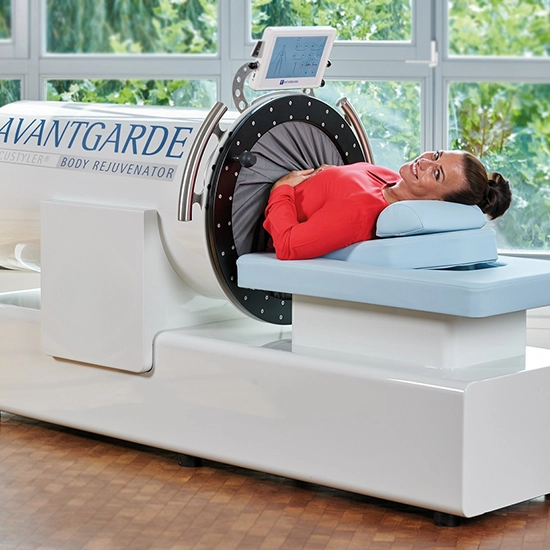
One of the primary methods used to support new vessel formation is hyperbaric oxygen therapy. In this treatment, pure oxygen is given to the patient under high pressure, increasing oxygen delivery to the tissues and stimulating angiogenesis (the formation of new blood vessels). In addition, biological methods such as growth factors and stem cell therapy contribute to new vessel formation by regenerating cells in the damaged area.
Endovascular interventions and surgical methods can also be preferred to improve blood circulation. For example, opening blocked vessels with balloon angioplasty or stent applications allows more blood to reach the tissues. Physical activity and exercise are important to strengthen existing vessels and improve capillary circulation. When applied with a multidisciplinary approach, all these methods enable successful outcomes in the treatment of diabetic foot.
Sixty percent of diabetes-related limb losses occur as a result of wounds on the foot becoming infected. Therefore, effectively treating infection is a critical part of diabetic foot management.
If the infection has spread and reached a life-threatening stage, broad-spectrum antibiotic therapy should be started immediately, taking into account the possible pathogens. However, if this is not the case, the most appropriate approach is to identify the infectious agent through tests performed on samples taken from the wound, and to plan treatment based on the pathogen’s antibiotic sensitivity.
Unfortunately, in many diabetic foot patients, unnecessary and excessive use of antibiotics that are not targeted to the pathogen is common. Over time, this leads to the development of antibiotic resistance in pathogens, making treatment more difficult.
In addition, kidney function is impaired in a significant proportion of diabetic patients, and the side effects of antibiotics can cause kidney failure. Moreover, diabetic patients often take multiple medications. For this reason, the interaction of any prescribed antibiotic with other medications must be carefully evaluated.
For all these reasons, when choosing an antibiotic, the infectious agent, the patient’s kidney function, current drug treatments, and other individual factors must be meticulously considered. With this approach, the effectiveness of infection treatment can be increased and side effects minimised.
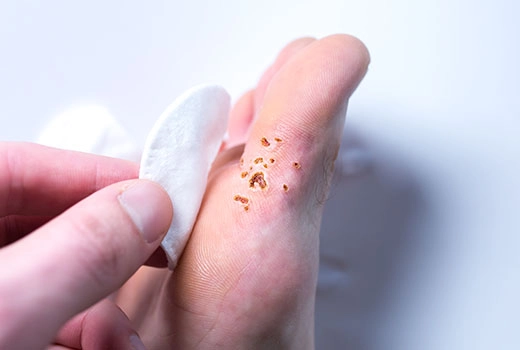

In diabetic foot ulcers, all dead and infected tissues must be removed. This procedure, called “debridement,” should be performed in a way that preserves the anatomical structure and healthy tissues, while allowing the patient to walk. Debridement can be carried out using sharp, biological, or chemical methods.
Sharp debridement should be performed by an experienced physician who is well-versed in foot anatomy. Since many diabetic patients have loss of sensation, they usually do not feel pain during debridement. However, for patients with prominent vascular problems, pain control is an important necessity.
During debridement, all non-functional tissues that hinder wound healing, including infected bones, are removed. The goal is to make the wound as clean as possible. Sharp debridement can be performed with traditional surgical instruments such as scalpels, curettes, and brushes, as well as with modern equipment such as ultrasonic devices or high-pressure water jets (e.g., Versajet®). By removing infected tissues, this procedure accelerates the wound healing process and helps prevent complications.
The wound healing process in diabetic patients is not the same as in healthy individuals and involves many challenges. Especially when blood sugar levels are high, the proliferation of cells responsible for wound healing stops, and these cells cannot regenerate themselves. This situation has a seriously negative impact on the healing process.
In the past, the belief that wounds in diabetic patients heal very slowly or do not heal at all was true. However, thanks to advancements in modern wound care products, this perception has largely changed. With the right treatment and appropriate product use, the healing process of diabetic wounds can be successfully managed.
That said, it is extremely important to correctly determine which product should be used for each wound. In addition, different products may need to be used at different stages of the healing process in the same patient. Therefore, careful assessment by specialists in wound care plays a key role in the success of treatment.
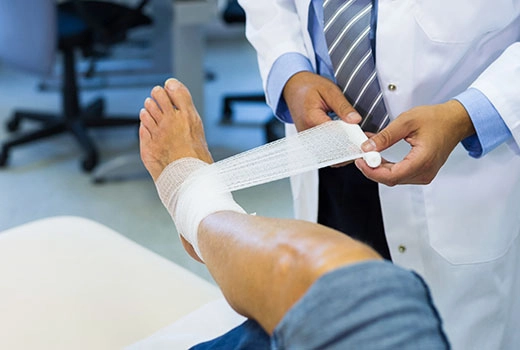
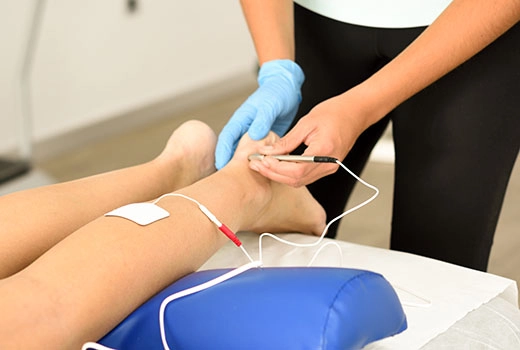
The main goal in diabetic foot ulcers is to prepare the wound for closure through reconstruction (repair).
For this reason, one of the most important stages of treatment is the reconstruction phase. While some wounds that are properly treated may close on their own during the treatment process, in other cases this process may take a long time or may not occur at all.
In such situations, reconstruction of the wound and foot may be required. This procedure is usually performed surgically, using methods such as skin grafts or tissue flaps. The aim of reconstruction is both to ensure rapid closure of the wound and to provide the patient with a functional foot that can bear weight.
One of the main goals of a chronic wound and diabetic foot clinic is to prevent the formation of new wounds on the feet of treated patients and to keep their health under control through regular follow-up. After treatment, it is very important to provide ongoing support to patients. In this regard, the clinic should offer the following services: